
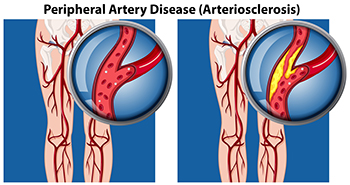
Peripheral artery disease, or PAD, can seriously affect the feet by limiting blood flow through narrowed arteries. This often causes pain while walking that eases with rest. As peripheral artery disease progresses, pain may continue even when not moving. Common symptoms in the feet include numbness, tingling, coldness, and skin discoloration. In some cases, one foot may feel significantly cooler than the other. PAD can also lead to slow-healing ulcers on the feet or toes, which may become infected and require prompt medical care. Skin on the feet may appear pale or take on a bluish tone, and toenail growth can slow or stop due to poor circulation. In advanced stages, tissue damage may occur, increasing the risk of limb loss, if left untreated. A podiatrist can help by identifying early signs of PAD and providing appropriate treatment to improve foot health. If you have symptoms of PAD that are affecting your feet, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Larry Cohen from New York City. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our offices located in Midtown, Manhattan New York, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.

Wearing proper safety footwear in the construction field is essential for protecting workers from common job site hazards. Puncture resistant soles help guard against sharp objects on the ground, while slip resistant materials reduce the risk of falls on wet or uneven surfaces. For long hours on the job, breathable materials and ergonomic design support comfort and reduce fatigue. Poor footwear can lead to muscle strain, joint pain, and spinal stress. A podiatrist can assist by addressing foot issues caused by wearing improper shoes, relieving pain, and offering advice on supportive footwear choices. If you have developed foot conditions from wearing the wrong shoes, it is suggested that you contact a podiatrist who can treat various foot issues, and guide you on the proper shoes to wear for your workday.
While working on the feet, it is important to take the proper care of them. For more information about working on your feet, contact Dr. Larry Cohen from New York City. Our doctor will treat your foot and ankle needs.
Working on Your Feet
Standing on your feet for long periods of time can cause stress and pain in your feet. Your whole body may experience change in terms of posture, back pain, bunions, callouses and or plantar warts. There are ways to avoid these conditions with proper foot care, smart choices and correct posture.
Positive Changes
Negative heeled shoe – Choosing this shoe type places the heel slightly lower than the ball of the foot. These are great for overall foot health. Find shoes that fit you correctly.
Go barefoot – Our feet were not designed to be enclosed for all hours of the day. Try to periodically expose your feet to air.
Eliminate Pain
Foot Exercises – Performing simple exercises, incorporating yoga and doing stretches are beneficial. This will allow increased blood flow to the area and muscles of the foot.
Achilles tendon – Stretching the foot out flat on the floor will relax the calf muscles and tendon. These exercises can be performed almost anywhere. Make sure you add these exercises to your daily regimen.
With a little bit of this information and knowing more about foot health, you will notice changes. Foot stretches and proper footwear will help with pain and prevent further issues.
If you have any questions please feel free to contact our offices located in Midtown, Manhattan New York, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
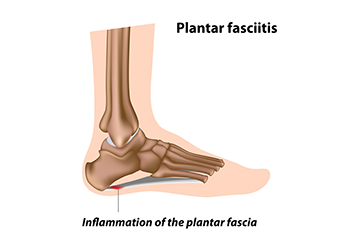
Plantar fasciitis is caused by inflammation of the plantar fascia, the thick band of tissue that runs along the bottom of the foot and supports the arch. This condition often leads to sharp heel pain, especially with the first steps in the morning or after long periods of rest. Risk factors include prolonged standing, flat feet, high arches, obesity, and wearing footwear that lacks proper support. Symptoms include aching, stiffness, or a burning sensation in the heel. If left untreated, the pain can become chronic and interfere with daily activities. A podiatrist can diagnose plantar fasciitis, provide targeted stretching exercises, and offer custom orthotics or treatments to relieve pain and promote healing. If you have heel pain, it is suggested that you consult a podiatrist who can accurately diagnose and treat the condition.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Larry Cohen from New York City. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Midtown, Manhattan New York, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.